Could the Food You Eat Be Affecting Your Rheumatoid Arthritis Symptoms?
Many of my clients with rheumatoid arthritis (RA) wonder if certain foods affect their symptoms, and some observe that diet affects their joint inflammation. Food may play a role in inflammation for some people with RA — but knowing which foods are involved can be confusing.
As part of my PhD research, I carried out a scoping review looking specifically at how elimination and reintroduction diets have been used to identify possible food triggers in adults with RA.
Here’s a summary of what I found, and how it might help guide your own nutrition journey.
What Is an Elimination-Reintroduction Diet?
An elimination-reintroduction diet is a structured way to explore whether certain foods are worsening symptoms such as joint pain, swelling, or fatigue.
It’s done in two phases:
-
Elimination: You remove foods that are most likely to be inflammatory or allergenic for a few weeks.
-
Reintroduction: You gradually bring foods back one at a time while watching for any changes in symptoms.
If a reaction appears when you reintroduce a food – and disappears when it’s removed again – that food might be a personal trigger.
What the Research Shows
Across 37 studies published between 1949 and 2024, researchers tested elimination-reintroduction diets and food challenges in adults with RA.
What Kinds of Diets and Challenges Were Used?
Most studies began with a short, very restricted elimination phase, which included one of the following approaches:
- Fasting protocols: water or juice only for 4–10 days, supervised in hospital or inpatient settings.
- Low-allergen replacement diets: a meal replacement plus a few hypoallergenic foods for about four weeks.
- Few-foods diets: highly restricted whole-food diets lasting one to four weeks, often allowing one or two protein foods (e.g. cod or lamb), a small range of vegetables, and one or two fruits, with mineral water only. Some versions were entirely plant-based.
- Single-food exclusions: for example, dairy-free diets.
Participants typically followed the restricted diet for at least a week. During this period, symptoms improved in around 70–80% of participants, though not everyone experienced benefits. Once symptoms improved, foods were reintroduced one at a time (or in groups), and reactions were observed by clinicians or the participants themselves. Reactions usually included joint pain, swelling, or stiffness, and some studies also measured laboratory markers of inflammation.
Foods were added back at varying intervals, some studies introduced three foods per day (five hours apart), while others tested one new food every two to five days. If a food caused symptoms, it was excluded again until symptoms resolved, after which another food could be tested. This process generally took four weeks to four months.
How Quickly Did Reactions Occur?
In six studies, researchers recorded how long it took for a reaction to appear.
Typically, reactions began within 1-48 hours, although 2-24 hours was most common in the case studies. Symptoms usually subsided within 24 hours to 10 days after the food was removed. This delay suggests that testing new foods every 2–3 days provides the most accurate results.
Interestingly, one study focusing solely on dairy found that participants developed joint swelling and pain only after two to three weeks of regular consumption.
In blinded food challenges, where participants did not know if they were receiving the suspected food or a placebo, some individuals still experienced worsened symptoms, suggesting a genuine physiological reaction.
A subset of participants identified foods that reliably triggered symptoms. By permanently excluding these foods, some achieved reduced disease activity, and a few were able to remain symptom-free and discontinue medication.
Which Foods Commonly Triggered Symptoms?
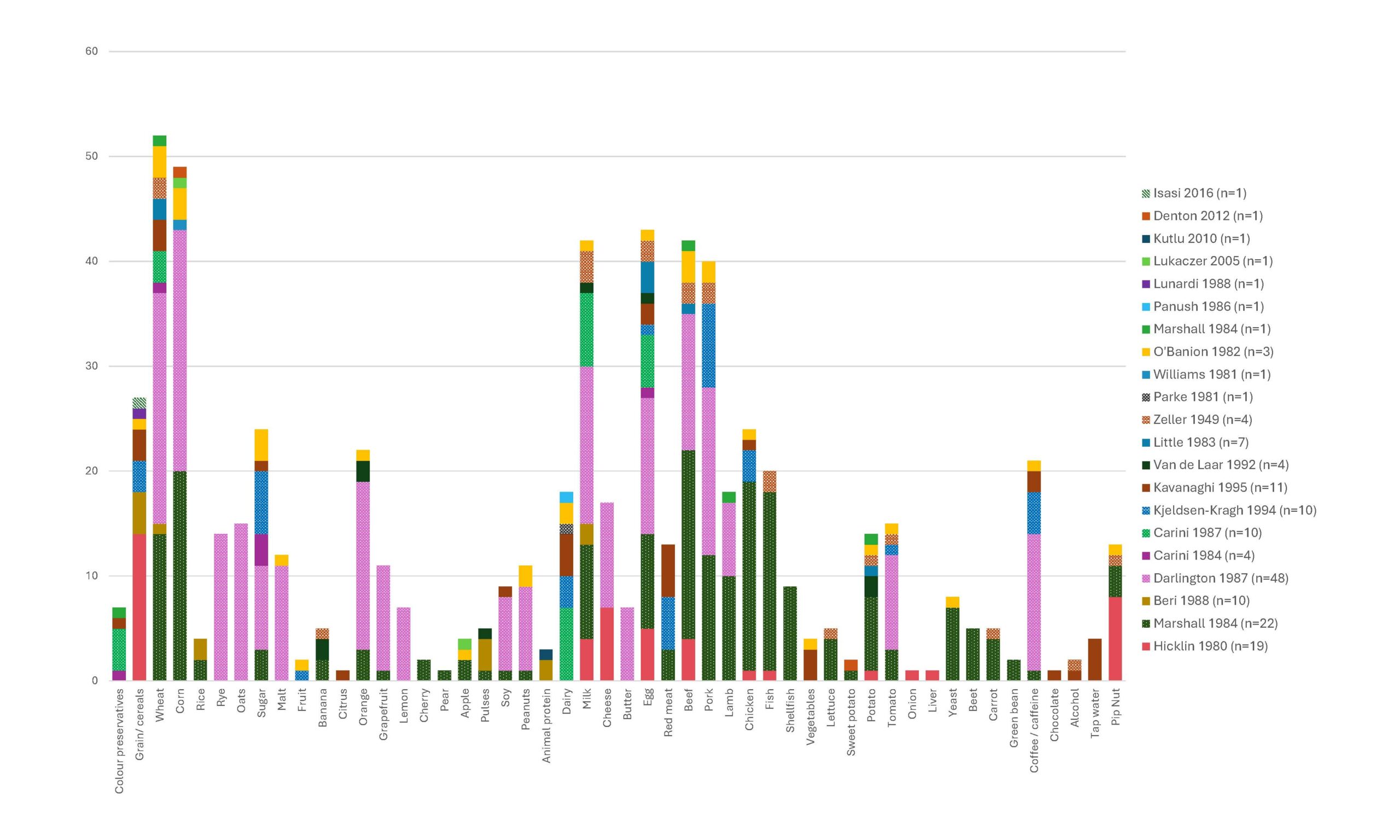
Ten studies and 16 case studies (involving 161 people) listed the foods that triggered symptoms and how many participants reacted to each.
When results were combined, the most frequently reported trigger foods were:
- Cereal grains: particularly wheat and corn
- Dairy products
- Eggs
- Beef and pork
- Nightshade vegetables: tomatoes and potatoes
- Sugar and caffeine/coffee
The graph below shows the cumulative food reactions from 161 people from all the studies that listed foods. AS you can see there are trends, however food reactions were also highly individual.
What This Means for You
At this stage, there’s no one-size-fits-all elimination diet for RA.
However, if you suspect food is influencing your symptoms, a carefully structured elimination-reintroduction plan can help identify triggers, and it’s safest to do this with professional support to ensure your diet remains balanced and nutritionally adequate.
Before considering an elimination diet
Before removing any food, I suggest starting with a with a nutrient-dense, anti-inflammatory foundation (lots of vegetables, quality protein, healthy fats). These diets without any specific eliminations improve symptoms and reduce inflammation. Key points are
- Increase fruit and vegetables
- Remove refined grains (white flour products, limit white rice)
- Remove free sugars (any sugar outside its natural package)
- Eat unprocessed foods without additives (processed meats, packaged processed foods)
- Focus on balanced meals with whole food – meats (lean meats are best) seafood, poultry, fruit, vegetables, nuts and seeds and cold pressed oils.
- Foods that improve the gut microbiome and reduce inflammation are fibre and colour rich plant foods (polyphenols and antioxidants), seafoods of all types for omega 3
If you do wish to test foods, I suggest removing the common trigger foods, as you see in the list above, rather than a very restricted diet.
- Remove suspected triggers for 3–4 weeks.
- Reintroduce foods one at a time while tracking symptoms and energy.
This process helps clarify which foods are truly problematic, versus those that are safe to include, and improving food quality often improves overall gut and metabolic health.
A Note on Current Diet Trends
You might have heard of diets like the Autoimmune Protocol (AIP) or the Paddison Program. Both have been popular among people with autoimmune diseases.
The AIP is a true elimination-reintroduction approach, while plant-based plans like the Paddison Program typically focus on exclusions without a formal reintroduction phase.
The Bottom Line
Elimination-reintroduction diets can be a valuable tool for people with RA, however they do need to be done thoughtfully.
The goal isn’t to eat less variety forever, but to understand your body’s responses and build a long-term, balanced eating pattern that supports joint health, energy, and wellbeing.
If you’d like guidance through this process, or want help creating a nutrition plan that supports your RA management, you can book a consultation or get in touch with me directly.
Here is a link to the full scoping review, where you will find a very detailed overview of the topic: Elimination reintroduction diets and oral food challenge in adults with rheumatoid arthritis: a scoping review
The supplementary data has details of all the studies investigated
An intervention using the AIP elimination-reintroduction diet is the other part of my PhD and results are currently awaiting publication.